
Which is worse? Flying a redeye, imbibing too much, or sleeping in the mountains? Surprisingly, it’s a tossup.
That’s because the “thin” air that characterizes Rocky Mountain towns has long-term health impacts on our sleep, hearts, brains and blood. These include effects we don’t typically hear about.
At high altitudes, air pressure decreases, making less oxygen available to us. When we first arrive or return to high elevations, whether after a vacation at grandpa’s house in Wisconsin, or on a weekend trip to A-Basin, our bodies immediately begin compensating for the “thinner” air. Our hearts beat faster and our blood pressure increases, as we labor to maintain adequate oxygen delivery to tissues. Eventually, our blood becomes more syrup-like as our bodies work to increase our blood’s concentration of oxygen-grabbing red blood cells. Sometimes we don’t acclimate well to these changes, like when we come up to elevation too quickly. Symptoms such as nausea and headaches result—often combining as acute altitude sickness, or even worse, leading to swelling of the lungs or brain.
Fortunately, most of our body’s systems, such as our blood chemistry and red blood cell counts, adjust within a matter of weeks to months.
But the critical things that don’t revert to normal are our breathing and our sleep.
At elevations above ~7500 feet (think: Estes Park), nearly everyone breathes faster and deeper. This behavior helps us get enough oxygen to satisfy our body’s needs. It also speeds up the rate at which we get rid of carbon dioxide, or CO2, a natural waste product of metabolism that builds up in our blood. The more CO2 in our blood, the more acidic it becomes.
This is where it gets interesting—because the main way our body determines how to breathe while we’re sleeping is by sensing how acidic our blood is.
Elevation wreaks havoc on this process.
When our nighttime blood becomes too acidic from CO2 buildup, our lungs are signaled to breathe more to expel this waste gas. But at high elevation, we get rid of CO2 more readily than at low elevation, leaving us with lower overall CO2 levels while we’re at rest. The situation is exacerbated while we’re in our most restful condition—sleep. While in this state, our “breathe” sensor isn’t triggered as much as usual, because our blood isn’t very acidic. As a result, our lungs are signaled to stop breathing for up to 15 seconds at a time. This causes oxygen levels to drop in our blood, brains and other tissues. That is, until our body recognizes the situation, and lurches back into rapid, deep breathing—a cycle called periodic breathing.
Physiological changes
Three physiological changes result from this high-stakes chain reaction. None of them go away, although mountain dwellers become desensitized to them over time.
First, periodic breathing interrupts our sleep and lowers our sleep efficiency. It reduces the amount of time we spend in slow wave sleep, a sleep that’s crucial for our bodies’ restorative activities, memory processing and hormonal regulation. Over time, the toll of this diminished sleep quality could be significant, yet most people who experience periodic breathing don’t even know they’re doing it.
Second, organs like our brains and hearts regularly experience reduced oxygen levels while we’re sleeping at high elevations. This oxygen stress inhibits their function, temporarily exacerbates acute altitude sickness, and can lead to long-term complications.
The third change is unrelated to periodic breathing, but can still be disconcerting. At higher elevations we urinate more because our kidneys sense our low blood acidity levels, and they respond by increasing their rate of excretion of a low-acidity compound called bicarbonate. Urination is how we rid our bodies of this bicarbonate. The temporary thickening of blood that occurs upon first arrival in the mountains is also caused, in part, by increased urination. That’s why dehydration is such a big issue for short-term mountain visitors.

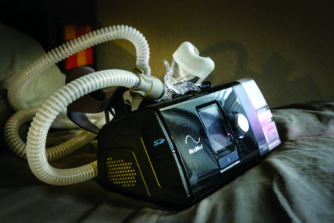
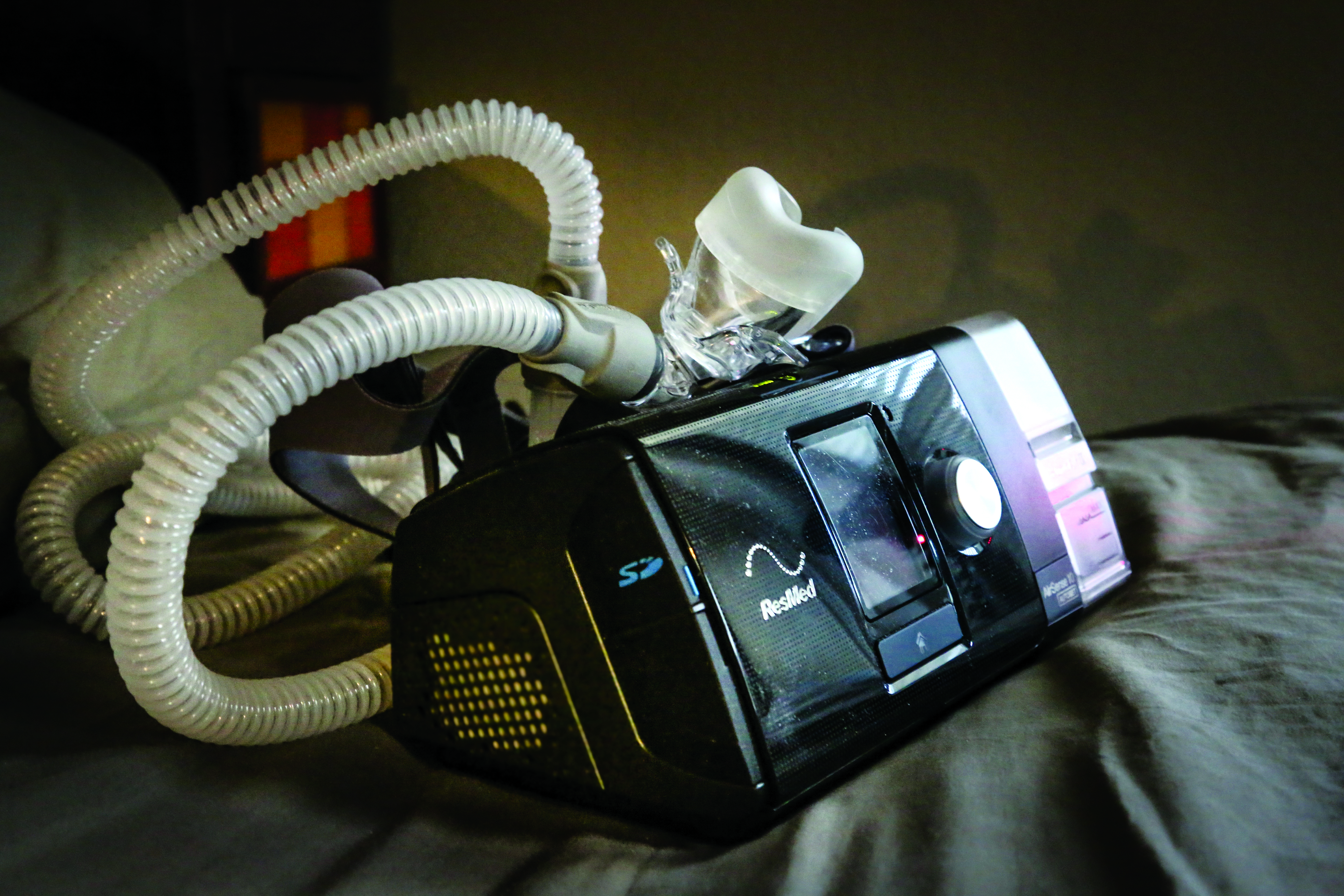
APAP (Automatic Positive Airway Pressure) machines push a prescribed amount of air in sleepers’ noses to maintain continuous breathing.
Are there solutions?
For short-term acute altitude sickness, the best bet is to descend to low altitudes or to avoid it by ascending to elevation gradually, while staying hydrated. To mitigate long-term altitude effects, some mountain denizens are sleeping with an oxygen concentrator. In severe cases, a doctor may prescribe acetazolamide; it tricks our body to breathe more by increasing the acidity of our blood. This ups our oxygen levels.
Sleep scientists are working in the lab and the field to find remedies. A key target? Studying the hundred million or so native peoples who’ve evolved over the millennia to live at high elevations in the Andes, Tibet and Nepal.
Look online for a graph showing how key metrics of sleep vary over a 30-second interval of REM sleep in a person sleeping at 10,800 feet.
James Hagadorn, Ph.D., is a scientist at the Denver Museum of Nature & Science. Suggestions and comments are welcome at jwhagadorn@dmns.org.

Excellent useful information. I since relocated to elevation 7,250ft coming from elevation 720ft