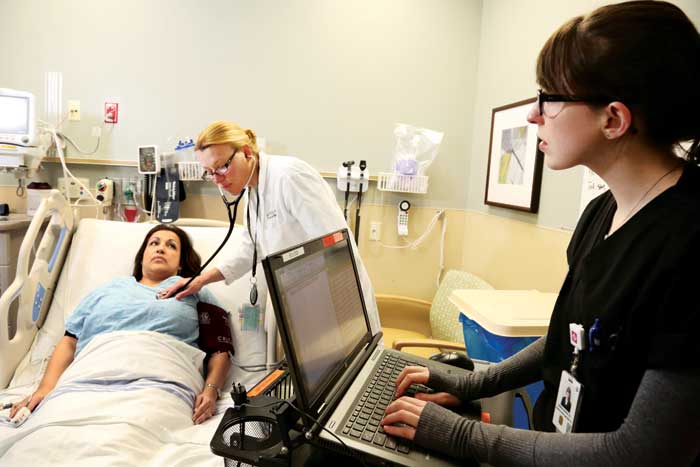
With community health worker Rene Ramirez filling in as a patient, director of the scribe program Dr. Jennifer Wiler and program manager Ashley Domin demonstrate how scribes record electronic charts at the University of Colorado Hospital Emergency Department.
Dressed in black scrubs and comfortable walking shoes, Ashley Domin follows a physician into a patient’s room at the University of Colorado Hospital (UCH) Emergency Department.
She wheels a cart equipped with a laptop. Like a fly on the wall, Domin listens as the doctor asks questions and assesses the patient. The doctor communicates what he or she finds. With incredible speed, Domin types the appropriate information into an electronic medical chart.
While Domin types away, the physician is able to give full attention to the patient. Once the evaluation is over, she follows the doctor into the next room, wheeling her mobile workstation.
Domin, 27, is a medical scribe, a relatively new field that is appearing in emergency departments and clinics nationwide. Medical scribes complete electronic medical records in real time—a relief for doctors and patients, especially in high-volume emergency rooms.
“Patients are happier because the physician is actually looking at them and sitting at the bedside and paying attention, rather than worrying about writing everything down,” she says.
Domin manages the scribe program at UCH. When the program started two years ago, there were only eight scribes, and they covered one third of the shifts in a day. Now the program employs more than 40 scribes, and they cover all but two shifts a day.
Domin will also manage the scribe program at Denver Health opening in April. As more hospitals and clinics switch to electronic systems, the number of scribes increases nationwide.
While electronic records have strong benefits—coordination among healthcare services, reduced medical errors, and more accessible information—many hospitals have resisted, but soon that will change.
Up until now, as part of the Affordable Care Act, hospitals have received reimbursement incentives to switch to electronic systems. But beginning in 2015, hospitals will face penalties.
Electronic systems are expensive, and practices have to change how they operate. A large amount of data has to be entered into the computer at a patient’s bedside or shortly afterward—a daunting task for doctors whose main focus is patient care, not paperwork.
A recent pilot study reports Kaiser doctors spend an average 30 to 40 percent of an overall shift sitting at a computer plugging data into charts, according to Kathleen Myers, chief medical officer and founder of Essia Health.
“That means they have to spend 20 minutes of every hour sitting in front of a computer; that’s 20 minutes they’re not seeing patients,” she says.
As an emergency physician, Myers recognized the need for support moving into electronic records.
In 2011, she founded Scribes STAT, an Oregon-based company that sets up scribe programs at hospitals nationwide, including UCH. In February, Scribes STAT was rebranded as Essia Health, which offers additional services for hospitals transitioning to electronic systems.
“What you notice is lots of happier doctors now,” she says. “When I get to work with a medical scribe, I get to sit on the stool and actually look at the patient and engage with him or her.” Now Myers only goes on the computer for a quick research question.
Emergency departments are relishing the many benefits of scribes.
With scribes, doctors are able to see more patients, which cuts down the patient wait time. Often 20 to 30 years old, scribes are generally more tech-savvy than older doctors and record details in real time, making charts more accurate. Scribes also update doctors on lab and X-ray results. Scribes do not help determine the right time for a patient’s admission or discharge. They do non-clinical duties like coordinating with family members in the waiting room, retrieving blankets for patients or giving directions to visitors.
Scribes make providers approximately 10 percent more efficient, according to Jennifer Wiler, MD, MBA, director of the UCH ED scribe program and vice chair of the Department of Emergency Medicine. The rough estimate is based on the number of patients treated in a certain amount of time, as well as the time it takes to fill out charts.
Scribes and doctors both benefit from the arrangement, according to Wiler.
“I’m getting a jumpstart into medicine,” says Ashley Domin, who intends to go to medical school. She first heard of scribing seven years ago when she saw a flyer in the science building of Wisconsin State University, where she studied biology.
Scribes are typically at the end of college or in a gap year between college and graduate school and interested in a career in medicine as a physician’s assistant or doctor.
With an 80 percent acceptance rate into medical school among scribes, Myers expects scribing will become a requirement to apply for med school in the future.
Domin has scribed in a family clinic and dermatology office—even more detailed coding. For two years, she worked as a traveling trainer and set up scribe programs at hospitals around the country. After seven years as a scribe, she continues to learn new terms all the time, and says billing and coding continues to be convoluted and overwhelming. But no part of the job has been as difficult as the training.
There is no national standard of how scribes are trained and credentialed. Each scribe company has a different training program. Trainees with Essia Health learn in a classroom setting. They are quizzed on medical terminology, and billing and coding, which are not taught in medical school but learned on the job.
“It’s like trying to take a drink out of a fire hydrant,” Domin says, remembering the overwhelming amount of information.
“You’re just doing your best, but essentially you’re learning what physicians had eight years to learn,” she says.
After passing the exam, trainees practice charting in a classroom and then one-on-one with a “super scribe,” or experienced scribe. They spend 80 to 100 hours with a super scribe.
Once hours are completed, a trainee is certified by a doctor and can begin scribing on his or her own. After practicing the technical aspects of a chart, scribes begin to think like a physician.
While listening and typing away, Domin thinks of each patient as a puzzle. She pieces together the symptoms and considers what tests, medication and blood work to order.
During a typical 8-hour shift at UCH, she sees about 30 patients. On her busiest day she saw 42. “It’s chaotic, but it’s a good chaos. You look up and suddenly five hours have gone by.” Recently, twice in one night she saw a thoracotomy—cracking open the chest to better view internal bleeding, the most memorable thing she has seen on the job.
Scribing has confirmed for Domin she wants to go to medical school and hopes to do emergency medicine or trauma surgery. Until then, she plans to continue as a scribe.

Great article. Very informative, and shows the personal side of the job and how that fits into the professional side.